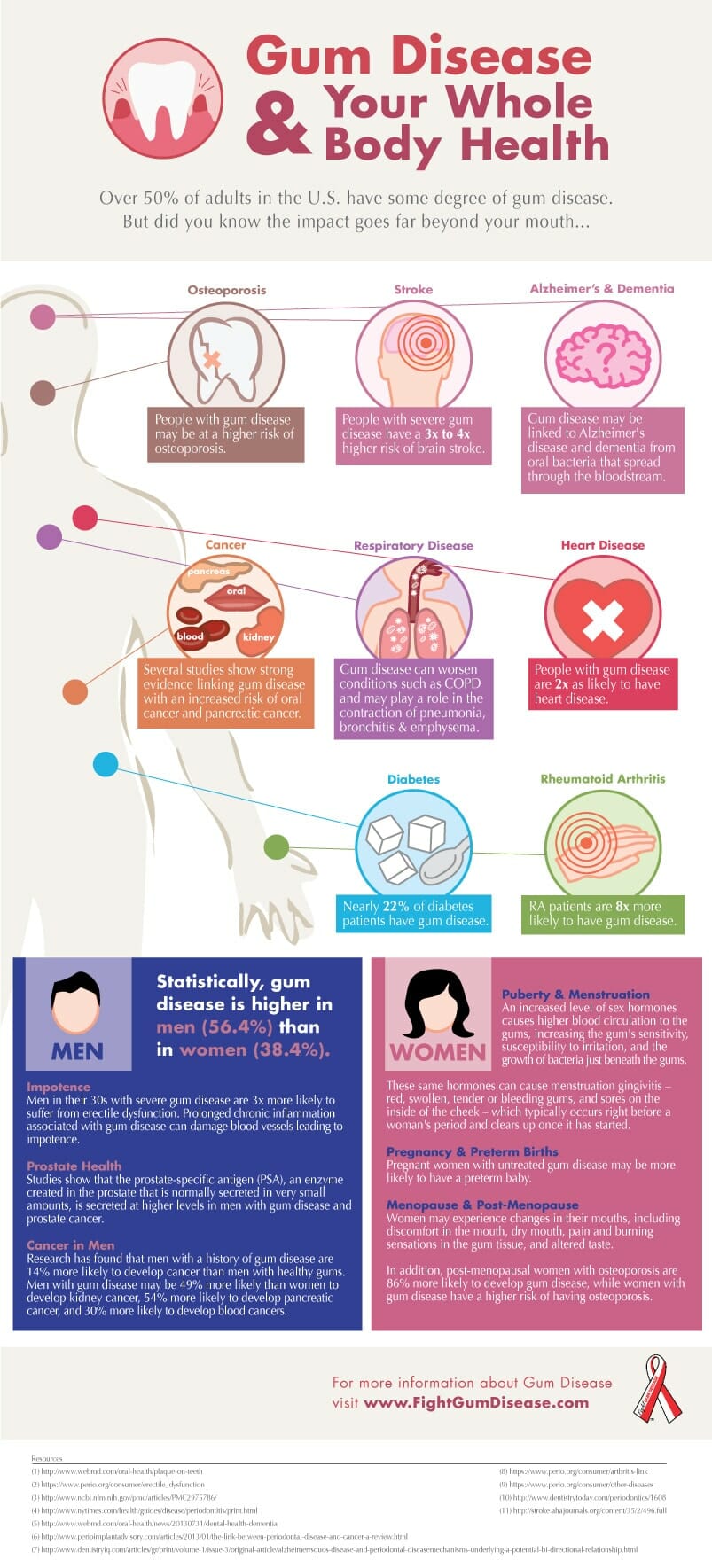
Did you know that periodontal disease can negatively impact the rest of your body? The bacteria that accumulate around your teeth can also find their way into the blood stream and circulate throughout your body.
The same germs have been found in a variety of tissues including the heart, brain, lungs, and even the placenta of pregnant women. To fight this invasion, that body produces an inflammatory response that can increase the risk for diabetes, heart disease, cancer, stroke, respiratory diseases and pregnancy complications.
More Information
Inflammation
Inflammation is the most likely link between periodontitis and other systemic diseases. The function of inflammation is to defend the body against microbial infection, and to repair injured tissues. But, inflammation does have the potential to cause harm.
Bacterial plaque around teeth can cause inflammation. Inflammation generally begins with an influx of plasma fluid (swelling) and defense cells (white blood cells). This creates a reddish halo around the gums, called gingivitis. The purpose of this is to eliminate microbes and clean out damaged tissue. If the plaque biofilm persists around teeth, inflammation can change into a chronic state, involving different, more specific defense cells.
Resolution of inflammation requires certain cellular mechanisms that trigger a “clean and repair” response. When those mechanisms are dysfunctional, inflammation can become a self-sustaining chronic condition, like periodontal disease. However, it is well known that not everyone is equally susceptible to developing periodontal disease. More importantly, many of the people that that show this inflammatory dysfunction may be susceptible to other inflammatory diseases.
Diabetes
Research has proven time and again that there is a very close link between periodontal disease and diabetes mellitus. Not only can poorly controlled Diabetes lead to a progression in periodontal disease, but untreated periodontal disease can increase the bodies’ inflammatory load making it more difficult to control their blood sugar.
Diabetes patients have a higher susceptibility to infection, thus are at greater risk for developing periodontal disease, even in patients with well-controlled diabetes. Increased sugar in the blood impairs the body’s defense system against infection, mainly the white blood cells.
Diabetes can also cause thickened blood vessel, making it harder for immune cells to travel to an area of infection. Even worse, diabetes also damages the collagen repair mechanism in our body, so the body has even more trouble healing from a wound. Uncontrolled diabetes allows all of these destructive effects to occur at an even faster rate.
On the other hand, periodontal disease has been shown to increase blood sugar. This allows greater periods of time when the body has to function with higher blood sugar. Bacterial infections, like gum disease, has a negative effect on the body’s metabolism. This makes it more difficult for the patient to consistently control healthy blood sugar levels. Periodontal disease may be a chronic infection, but its’ effects increase the risks of many the complications of diabetes: glaucoma, neuropathy, high blood pressure, stroke and many others.
The good news is that evidence shows that periodontal therapy helps! Treating periodontal disease may help prevent complications of diabetes by helping maintain your blood sugar. Recent evidence suggests treating periodontitis can decrease HbA1c% by approximately 0.4%.
Maintaining oral health allows you to better control your blood sugar. If you or someone you know has diabetes, we urge you to schedule an appointment today to test for periodontal disease.
Cardiovascular Diseases
Experts agree that periodontal disease increases the risks of the following atherosclerotic cardiovascular diseases (ACVD) and their events:
- Coronary Heart Disease which presents as angina or heart attack
- Ischemic Cerebrovascular Diseases such as stroke or mini-stroke (transient ischemic attack or TIA)
- Peripheral Vascular Diseases such as deep vein thrombosis
This risk association has been demonstrated independent of other well-known cardiovascular risk factors such as smoking and diabetes. It is thought that periodontal bacteria and the by-products leak into the circulation through periodontal pockets. This initiates a chronic inflammatory response in the bloodstream which promotes development, maturation and instability of fatty lesions (atheroma) in the arteries leading to an ACVD event. In addition, multiple studies prove the existence periodontal pathogens, viable and non-viable, within atheroma in all locations in the body. Also, anti-bodies that normally fight these bacteria can cross-react with the cells lining the arteries and other blood-borne compounds, perpetuating the inflammatory process.
Thankfully, periodontal therapy has been shown to reduce the overall level of inflammation within the circulation, as shown in the reduction of a number of biomarkers such as C-reactive protein, endothelial cell function, blood clotting ability, and arterial blood pressure among others. It is widely accepted among health professionals that periodontal therapy, along with improved oral hygiene, can help reduce overall systemic inflammation and should be part of a patients plan toward improved cardiovascular health.
Pregnancy
Expectant mothers know a healthy lifestyle is important for her and her baby. Periodontal health is just another part of the picture. Research indicates that women with periodontal disease may be at risk for adverse pregnancy outcomes such as preeclampsia, pre-term delivery and low birth-weight babies, and even other more severe conditions. Again, the common link is bacterial-related inflammation. The concern is that bacteria and inflammation that enter the bloodstream can eventually reach the placental membranes, amniotic fluid and the umbilical cord.
The recommendations from the American Academy of Periodontology state that non-surgical periodontal therapy is perfectly safe for pregnant women and may aid in improving periodontal health. The American College of Obstetricians and Gynecologists agree that sustained oral health is vital and the recommend regular dental visits during pregnancy.